Continuous Glucose Monitoring Training in Cullman, AL
you’re ready to move beyond finger pricksContinuous glucose monitoring (CGM) is a powerful tool for people with diabetes. These small, wearable devices track your glucose levels day and night, providing real-time data to help guide treatment decisions. Whether you’re managing type 1 or type 2 diabetes, learning to use your device properly is key to success.
At Cullman Diabetes Center, our hands-on CGM training walks you through everything from sensor insertion to interpreting your glucose trends. We’ll help you feel confident, comfortable, and supported as you make the switch to this advanced diabetes technology.
How Do Continuous Glucose Monitors Work?
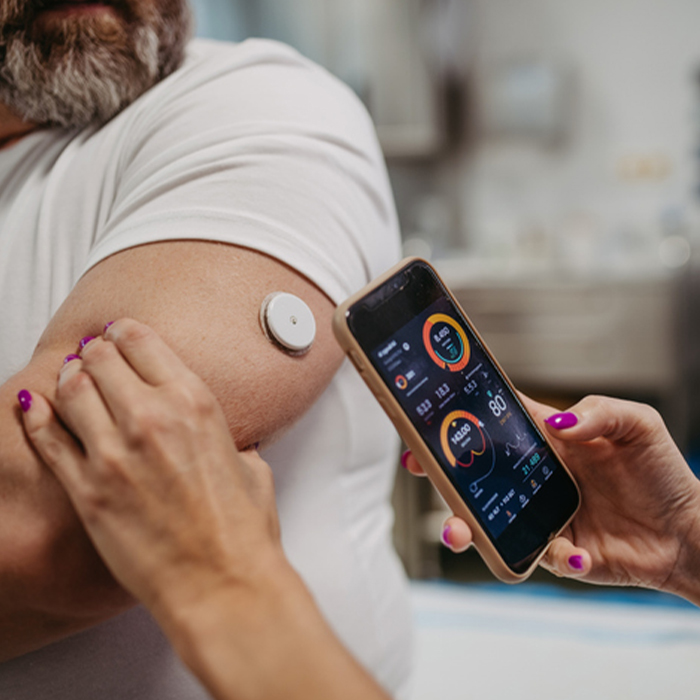
Hands-On Help From Experienced EducatorsCGMs use a small sensor placed under your skin, usually on your abdomen or upper arm, to measure blood glucose levels in real time. A transmitter sends the data to a reader, smartphone app, or insulin pump, depending on the model. Many CGM sensors alert you to dangerous highs or lows before they become emergencies.
During your training, we’ll guide you through:
We’ll also compare continuous glucose monitoring vs. finger-prick testing so you understand the benefits and when traditional checks might still be helpful.

Get Help with Insurance, Prescriptions, and Access to CGM Systems
Curious about coverage and access to CGMs? You’re not alone.
We’re here to simplify the process and help you take the next step toward better blood glucose control.
FAQs About Continuous Glucose Monitoring Systems
Most CGMs are inserted with a small, spring-loaded applicator. The sensor is placed just beneath the skin, typically on the upper arm or abdomen. It’s quick, simple, and typically causes minimal discomfort.
Most sensors are approved for 7 to 14 days, after which they need to be replaced. Your trainer will show you how to track wear time and when to switch sensors.
Insertion may cause mild discomfort, but most users say it’s far less painful than finger pricks. After placement, most people forget it’s even there.
If you’re nervous, our educators can walk you through the process and help you feel at ease.
Yes, most CGMs are still prescription devices, especially those that integrate with insulin pumps or are used for intensive diabetes management.
In 2024, the FDA approved the first over-the-counter system, designed to provide continuous glucose monitoring for type 2 diabetes to those who are not using insulin. That means some people, including people without diabetes, may now access basic CGM technology without a prescription—but features may be limited.
If you’ve been diagnosed with diabetes, our team can coordinate with your primary care provider or endocrinologist to help you get started with a prescription device that meets your needs. We’ll also walk you through any insurance questions, including Medicare coverage options.
Yes! Most CGMs are water-resistant and designed to stay on during everyday activities like showering, swimming, or working out. Just be cautious of prolonged submersion or activities that could loosen the adhesive.
We’ll teach you how to protect your sensor and extend wear time without compromising comfort.
While CGM devices reduce the need for finger sticks, you may still need to check your blood glucose manually in some situations, such as when your symptoms don’t match the CGM data, during device warm-up periods, or if your CGM requires occasional calibration.
Your training session will cover when and how to double-check with a traditional blood glucose meter.

Take Control with Real-Time Glucose Insights
Let’s make sense of your numbers together. Learn how to use your continuous glucose monitor with support from experienced educators who care.